Our Services
Maternity
Our maternity service provides excellent care for more than 6,000 women a year.

We offer great facilities, pride ourselves on the individual care and attention each woman and family receives and we promote a philosophy of normal and natural labour and childbirth and midwives support women to achieve this.
If you need more specialised or complex care, our medical team of 15 dedicated and experienced consultants will ensure you have the best birthing experience possible.
Trust your instincts: Call your midwife or our maternity unit if you are worried.
Service moves across the Royal Bolton Hospital
- M2 (Antenatal) has moved to G3
- The postnatal ward has moved to G4
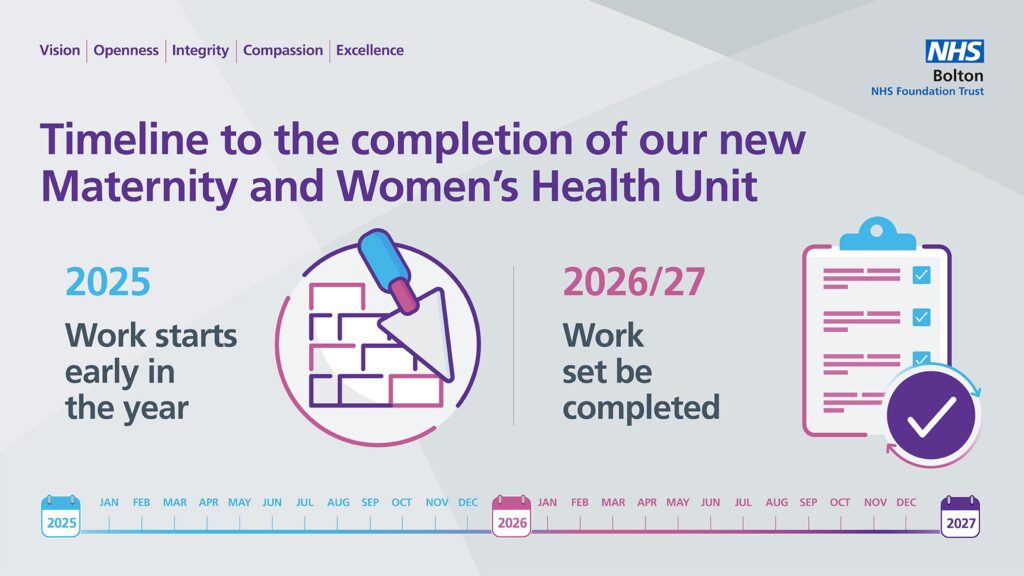
The Maternity and Women’s Health Unit at Royal Bolton Hospital is undergoing a multi-million pound transformation, which will include new birthing rooms and triage area, and upgraded assessment areas in our gynaecology services
The unit will be located at the current Princess Anne Maternity Unit, in M block of the hospital. Once complete, the unit will include:
- A new birthing suite with four brand new, modern birthing rooms with pools.
- A new seven-bed triage area.
- A new gynaecology and early pregnancy unit with modern standards and models of care.
- New transitional care bays for Neonatal services (within postnatal ward).
- Remodelled and refurbished maternity wards for women during and after pregnancy into new, modern and spacious environments.
- New modern façade/cladding to the building with new windows and doors.
The development is being funded by NHS England following the identification of reinforced autoclaved aerated concrete (RAAC) in the maternity unit in December 2023.
Since then, we have moved maternity services away from the affected areas to allow the areas to be propped for safety, with women’s services operating from new locations at the hospital and at Lever Chambers Centre for Health.
Once the development is complete, all maternity and women’s services will once again be located in M block.
Latest updates – March 2025
- Enabling works are now completed and we are excited that the ground-breaking for the development will happen very soon.
- The first work will be in maternity theatres.
Whilst the work is ongoing, there will be some reduction in parking spaces and road access disruption. This will be carefully managed by the project team to ensure that you always have a safe route into the maternity unit.
Your pregnancy and birth
We know that pregnancy can be an exciting but daunting time for women and their partners. There are many choices to make and questions to answer and we want you and your family have the best possible experience at this special time.
We understand how important it is to have support during pregnancy, and welcome:
Inpatient wards (M2, M4, M5)
- On the postnatal (now on G4) and antenatal (now on G3) wards two adult persons may visit at any one time between 9am-9pm.
- The two adult persons may change over.
- No more than two adult persons should be present at the bedside at any one time.
- Other children/siblings may visit during the postnatal period between 2-7pm, but must not be left unaccompanied at any time.
Visitors may be asked to leave the ward if privacy is required for an intimate examination or consultation.
M4 and M5 have been temporarily relocated within the hospital to G3 & G4 Wards.
Birthing areas
- Two named adult persons per woman may provide support at any one time before and during birth.
- After delivery the two named persons may change over when the ‘golden hour’ after birth has been completed and when the woman is ready to receive guests.
- No more than two adult persons should be present at the bedside at any one time.
- Other children/siblings may visit during the postnatal period between 2-7pm, but must not be left unaccompanied at any time.
During your pregnancy you will be offered regular appointments with a midwife or obstetrician. They check that you and your baby are well, give you support and information about your pregnancy to help you make informed choices.
If you have a positive pregnancy test or have recently moved to the area, here’s what to do next.
Get in touch with your local midwifery team as soon as possible to let them know about your pregnancy on 01204 390023. We will then contact you to schedule a first (booking) appointment with one of our midwives.
The NHS pregnancy and baby guide is a comprehensive source on all stages of pregnancy and what you can expect from NHS services. It will tell you how to work out your due date, gives a week by week guide and information on the early days, pregnancy (antenatal care), health and wellbeing, tests scans and checks, vaccinations, twins, common pregnancy ailments, pregnancy-induced conditions, existing health problems and preparing for the birth.
Our fabulous midwives work in teams across all parts of Bolton, Bury and Salford. You will see them throughout your pregnancy and after you give birth. Appointments may be held in children centres, Ingleside Birth Centre and hospital-based clinics.
Midwives may also visit you in your own home, especially after you have had your baby. If you live outside of our catchment area and want to have your baby at the Princess Anne Maternity Unit, you will be asked to come to the hospital to see a midwife here, but will also receive community-based care from midwives attached to your local hospital.
Our maternity services are proud to support you and your family to plan care that is individual to you while taking into account what is most important to you. We support your decision-making with robust, evidenced-based recommendations to help keep you and your baby as safe as possible.
Sometimes you may require enhanced support, time to understand the options before you, or to discuss your preferences for care. Our senior midwives run birth choices clinics at both hospitals to help this process, with the support of our obstetric colleagues.
If you would like to discuss your care options further, please talk to your midwife who can refer you to the clinic.
We’re really proud here in Bolton to be a trust that offers families the ability to have whichever birth they choose.
There are Maternity Choices for where you could give birth.
They are:
- at home with support from our midwifery team
- at Ingleside Birth and Community Centre, our midwife led unit in Salford (Unfortunately, Ingleside is currently unavailable as a place of birth)
- at the Royal Bolton Hospital delivery suite, our doctor led unit at the hospital
Speak to your community midwife to discuss which option is best for you during your next appointment. You can change your chosen place of birth at any point during your pregnancy by discussing it with your midwife.
Ingleside Birth and Community Centre
*Unfortunately, Ingleside is currently unavailable as a place of birth.*
Ingleside is set in a beautiful setting within Oakwood Park, Salford. Ingleside offers low risk women a unique birthing experience in a setting surrounded by nature in the heart of the community.
Would you like your care to be provided in a ‘home from home’ environment under the care of highly experienced midwives? Ingleside houses four spacious en-suite birthing rooms, each decorated with a modern and homely feel, with large, under lit birthing pools, dimmable mood lighting, Bluetooth speakers and flat screen TVs.
Feel free to contact us for a tour of Ingleside birth centre or for an informal chat with our team by calling us on 0161 357 1006 or ingleside@boltonft.nhs.uk.
What to bring with you
As you approach 36 weeks of pregnancy, we encourage you to start packing a bag ready for you and your baby regardless of where you are planning to give birth. You will normally stay in hospital from six hours to two days following the birth of your baby—therefore you need only bring enough clothes and other personal items for this length of time.
If you stay longer you can ask friends or relatives to bring extra things for you. Whatever you decide to bring is your personal choice.
We have put together some suggestions below.
For you
- Any hospital notes, a copy of your birth plan and list of contact telephone numbers
- An old t-shirt for labour or any comfortable clothing
- Pair of socks for labour
- Personal items—toiletries, tissues, tennis ball or wooden massager, massage oils, pillow, water spray, lip salve
- Toiletries including soap, toothbrush, toothpaste and lip balm
- Hair bands or clips for long hair
- Snacks, magazines, newspapers, puzzle books
- Breast pads
- Maternity pads and disposable knickers
- Towel
- Support bra to wear while breastfeeding
- Dressing gown, slippers, nightwear
- Comfortable clothing to go home in
Note: Please leave painkillers at home. We normally prescribe paracetamol and ibuprofen. Please ensure you are not allergic to or have any sensitivities to these medications before taking them.
For your partner
- Comfortable clothing and a change of clothes
- Suitable indoor footwear
- Toiletries
- Meals and snacks (please note only mothers receive hospital meals in the maternity unit)
- Change for the carpark
For your baby
- Baby grows or gowns—baby grows are the best for warmth and comfort
- Vests and cardigan
- Hat
- Baby bath towel
- Nappies
- Cotton wool
- Baby blanket
The main purpose is to medically examine you and your baby.
- The room will be dark and quiet to allow the sonographer to concentrate
- The screen will be facing the sonographer while the scan is being done. You will be able to view your baby once all checks are complete
- We check the pressure of the baby’s heartbeat during the scan, but you will not be able to hear it
- If we detect a problem with your baby, we will talk to you about this at the end of the scan
- Taking photos is not allowed – please do not attempt to do this a any point
You will be able to purchase photos for £5 after your scan. Your BMI and babies’ position could affect the quality of the image.
If your pregnancy has been uncomplicated and you are having a hospital birth, it is advisable that you stay at home for as long as possible during the early stages of labour, as long as your baby is moving and you are coping with the contractions. Evidence suggests that your home environment will encourage you to remain relaxed and therefore more able to cope with the pain.
Remember to continue to eat and drink during this time. Please telephone your midwife if:
- you think your waters have broken
- your contractions are becoming more painful and regular and you need midwifery support
- you have experienced any blood loss
- you have any concerns about the movements of your baby
- you have any other concerns
From time to time it may be necessary for our maternity team to enlist the support and advice of local social service teams. We will do this in order to ensure the safety and wellbeing of mothers and their unborn or new born babies. Usually these referrals are made with the full consent and cooperation of women and their families.
Safeguarding is a way of protecting people from harm, abuse and neglect. As with all of the health services we provide, your welfare and that of your baby is our highest priority. We will do all that we can to make sure that you both receive the support, compassion and care that you need.
Our specialist midwives are a vital part of our team and they may be involved in your care throughout, depending on your needs.
Our specialist midwives specialise in;
- Diabetes
- Mental Health
- Antenatal Screening for you and your unborn
- Breastfeeding team
- Specialist Liaison Cultural midwife and Bereavement care.
If you are less than 16 weeks pregnant and experiencing issues or have any concerns, please call our Early Pregnancy Assessment Unit to speak to our specialist nurses on 01204 390510.
Available 24 hours – 7 days a week.
Please visit our Gynaecology page for more information.
Your midwife will discuss the education we offer at your first appointment to ensure it is right for you.
We also encourage our patients to visit the following website for general antenatal education. This website provides one place to access information about maternity providers in your area.
Skin-to-skin contact is where a baby is dried and laid directly on your bare chest after birth.
However you plan to feed your baby, skin to skin after birth is the ideal way for you to start to get to know each other. In the first few hours after birth, holding your baby in skin to skin will help them to adjust gently to life outside the womb and support you both to begin a close, loving relationship. This benefits a baby’s brain development by reducing stress.
We will encourage you to hold your baby in skin to skin for at least the first hour after birth, and for you to give the first feed during this time. However you choose to feed your baby – they will all benefit from this experience.
Skin to skin contact can benefit you and your baby throughout the first year and beyond. For more information visit meeting your baby for the first time.
If you had your baby at home
If you had your baby at home and there are no complications, you will stay at home. Your midwife will make you comfortable, complete any documentation and give you emergency numbers to call before leaving. Your midwife will then arrange to visit you again soon.
If you had your baby at Ingleside Birth Centre
If you birthed your baby at Ingleside, then providing that you and your baby are well then you will stay at Ingleside for up to 6 hours. The midwife caring for you will conduct an examination of yourself and your baby and then you will be discharged home.
If you had your baby in hospital
If you had your baby in hospital, immediately after the birth you will be made comfortable either on the birth centre or labour ward. Your baby will be examined by your midwife. After an hour or so, you and your baby will be transferred to the postnatal ward or, if you are returning home straight from the birth centre, this will be encouraged after 3–6 hours.
If you have a Caesarean section or complicated instrumental birth you will be transferred to the recovery unit for close observation over the first 2–6 hours. When your condition is stable you will be transferred to the postnatal ward.
Before you leave
We will:
- Give you a postnatal check to ensure you are recovering well and are safe to leave
- Give your baby a paediatric check, including a hearing screening test
- Offer a BCG vaccination to your baby
- Give you leaflets, details of follow-up appointments and any medication you may need
- Give you a wave goodbye and check if you have any more questions before you go
You will:
- Need to ensure you know how you are travelling home with your baby, including bringing an appropriate car seat if taking your baby home in your vehicle
You will have a midwife assigned to your care to regularly review you and your baby’s progress. When it is time to go home, s/he will arrange your discharge.
Who will be involved in my care?
- Midwives: once you have been transferred to the postnatal ward, the ward midwives will plan your care, carry out your postnatal checks, give you advice and arrange your discharge from hospital.
- Physiotherapist: will provide you with exercises to aid your recovery
- Health Care Assistants: will assist and support you with breastfeeding, work closely with the midwives and perform routine observations.
- Maternity Support Workers: will look after you and provide you with support—such as learning new skills in caring for your baby—under the guidance of midwives.
- Medical staff: will be on hand if they are needed. Your baby will be examined fully in the first 24 hours of life by a neonatologist or midwife before leaving hospital.
- Neonatal Hearing Screeners: a first hearing test is usually conducted on babies before you go home. The screeners come to the ward every day and will undertake this test for your baby before you leave.
- Neonatal Team: will provide care to your babies if they need additional reviews or further support.
Screening tests for you and your baby provides information about the screening tests offered during and after pregnancy.
The animation is also available with subtitles and British Sign Language. Subtitled versions include English and translations in Arabic, Bengali, Chinese, French, Latvian, Lithuanian, Polish, Portuguese, Punjabi, Romanian, Somali and Urdu.
STFYAYB provides more information about the screening tests offered during and after pregnancy.
Caring for women and families within maternity services is our priority and often involves an examination, medical procedure and or an investigation/screening procedure.
Prior to any of these being undertaken the health care professional will use the latest information to discuss with you why we recommend this to be taken and what will happen during the procedure.
Your consent will be requested prior to each procedure even if you have undertaken the same procedure before.
No procedure will be undertaken without your consent however minor this may be. For some procedures this will be obtained verbally and for other procedures this will be taken by asking you to sign a consent form.
Informed consent may be taken at the time of the procedure or several hours, days or weeks before. If new information or your medical needs change before the procedure commences we will discuss this with you and seek your consent again.
If you are unsure of the information provided or wish to receive additional information, please ask the midwife, doctor or health professional to discuss this further. On some occasions the health care professional will also inform you of additional procedures that may be required during the procedure itself and ask you to consent to these being undertaken in advance.
For example, when planning a caesarean section advanced consent would be requested to undertake unplanned emergency procedures in the event you are unable to consent due to general anaesthesia or lack capacity.
In the event an emergency procedure was required and you had not previously consented to additional procedures a senior doctor would act in your best interest and undertake necessary procedures to prevent you from serious harm or death.
Pregnant women in Bolton are being invited to be vaccinated against Respiratory Syncytial Virus (RSV) for the first time in NHS history.
Maternity teams at Bolton NHS Foundation Trust are offering drop-in clinics for women who are over 28 weeks pregnant and have not yet been vaccinated on the following days:
- Monday – Crompton Health Centre – 10am-3pm
- Wednesday – Antenatal Clinic – 9am-4pm
- Thursday – Antenatal Clinic – 9am-4pm
- Friday – Antenatal Clinic – 9am-4pm
Please email MaternalVaccinations@boltonft.nhs.uk if you have any queries
Please fill out Maternity RSV Vaccination Referral Form as soon as you can, so we can find the best date for your vaccine.
For more information about vaccines during pregnancy, visit: https://www.nhs.uk/pregnancy/keeping-well/vaccinations/
North West Maternity Safety Information provides key safety messages in 12 different languages.
Some of the key message themes are:
- If you are pregnant and Black, Black British or Asian, Asian British – you might be more vulnerable.
- Trust your instincts – call your midwife or maternity team anytime if you are worried about your pregnancy.
- Is your mood ok? Who to speak to if it is not ok.
- What to do if you miss an appointment.
- Signs of labour and what to do if you think you are in labour.
- What to do if you have signs and symptoms of pre-eclampsia.
- The importance of taking Vitamin D.
- Feeling safe in your own home and how to find support if you don’t.
- Looking after you and your unborn baby.
- Follow us on Facebook
- Count the Kicks
- Dads Matter
- Lullaby Trust who provide advice regarding Safe Sleeping of a new born baby
- North West Maternity Safety leaflet
- Mybirthmychoice
All babies must be registered with the Registrar of Births, Deaths and Marriages within 42 days of the birth.
If you are married, either parent may register the baby.
If you are single, you are responsible for registering the baby. If you are single but you want your partner’s name to appear on the birth certificate, your partner must be present with you at the time of registration.
You will be given more detailed information on where and how to register your baby by a member of our team.
What is induction of labour?
Labour is a natural process that usually starts between 37 and 42 weeks of pregnancy. It is sometimes necessary to start the process of labour artificially. This is known as induction of labour.
Every year, approximately a third of women in the UK have their labour induced. Induction of labour is only recommended when it is thought it will benefit the health of you or your baby.
Please see Induction of Labour leaflet for more information.
Service locations
Ingleside Birth and Community Centre
At home - Speak to your midwife for more information
Key contact numbers
Maternity Scan
Tel: 01204 390915
Community Midwives’ Office
Tel: 01204 390023
Antenatal Clinic
Tel: 01204 390574
Maternity Triage
Tel: 01204 390612
Central Delivery Suite
Tel: 01204 390579
Ingleside Birth and Community Centre
Tel: 0161 357 1006
Early Pregnancy Assessment and Urgent Care
Tel: 01204 390510
Always call 999 in an emergency
Meet the team
Dr Nadia Ali-Ross
Consultant Obstetrician and Gynaecologist
Mr Prasanta Chattopadhyay
Consultant, Obstetrics and Gynaecology
Dr Sangeeta Das
Obstetrics and Gynaecology
Dr Judith Kundodyiwa
Consultant, Obstetrics and Gynaecology
Miss Khashia Khanam Mulbagal
Consultant, Obstetrics and Gynaecology
Dr Andrew Muotune
Consultant, Obstetrics and Gynaecology
Dr Neeraja Singh
Consultant, Obstetrics and Gynaecology
Dr Nahid Siraj
Consultant, Maternity and Gynaecology
Dr Bim Williams
Consultant, Obstetrics & Gynaecology